Slipped disc
A slipped disc occurs when a pliable cushion of tissue between the bones in your spine pushes out and often puts pressure on a nerve. Other medical terms used to describe this are a herniated, ruptured, or prolapsed disc. The most affected area is the lower back as this is a highly mobile region of the spine and therefore more vulnerable. But any disc can rupture and become herniated, including those in your neck.
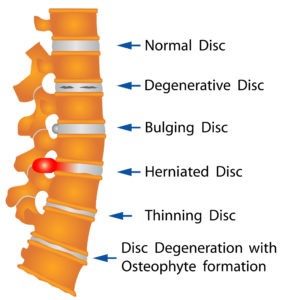
As we get older, our discs show signs of wear and tear. Over a period of time discs can dehydrate and stiffen up, causing the outer layer to bulge. You can also have a herniated disc, which is when your disc cracks in the tough outer layer of cartilage and allows some of the softer inner cartilage to protrude out of the disc itself pressing on the nerve.
What causes a slipped disc?
A slipped disc is usually the result of ageing and gradual wear and tear (known as disc degeneration). As you get older, your discs become less flexible and more prone to tearing or rupturing with even the slightest movement. It is hard to pinpoint the cause of a slipped disc; apart from age it could happen when lifting heavy objects.
The risk factors to take into consideration include:
- Weight – carrying excess weight causes stress on the discs in your lower back
- Occupation – demanding jobs have a greater risk of back issues, especially if they include repetitive lifting, pulling, pushing, and carrying heavy objects
- Genetics – You can inherit a predisposition to developing a slipped disc
- Smoking – Smoking lowers the oxygen supply to your discs, causing them to break down more easily
What are the early signs and symptoms of a slipped disc?
Presenting symptoms that indicate a slipped disc include:
Slipped disc in the neck:
- Numbness down one or both arms
- Tingling down one or both arms
- Weakness down one or both arms
- Pain in the shoulder, neck, or arm(s)
- Pain on neck movements
Slipped disc in the low back:
- A pain down the back of each leg from the buttocks to the knees (one or both legs)
- Numbness down one or both legs
- Tingling down one or both legs
- Weakness down one or both legs
- Pain in the buttocks, back, or legs
- Numbness and tingling around the anus *
- Some difficulty controlling your bladder and bowel *
*These may be considered as a medical emergency the symptoms are new. They may need immediate attention.
How is a slipped disc diagnosed?
Your doctor will ask you about your symptoms and examine you for signs of a slipped disc. They will also take your medical history and ask about your injury. X-rays do not detect slipped discs but can show arthritic changes in the joints. You will probably be sent for an MRI scan to confirm your diagnosis.
Your doctor will also perform various neurological tests to check the following:
- Reflexes
- Muscle strength
- Walking ability
- Ability to feel light touches or pinpricks
How is a slipped disc treated?
There are various ways to alleviate your pain and get you on the road to recovery as soon as possible. These include:
- Pain medications
- Cortisone injections
- Muscle relaxant tablets
- Opioids
- Anti-inflammatory medication
- Physiotherapy
- Stretching and strengthening exercises
- Hydrotherapy
- Massage
- Ice and heat therapy
- Electrotherapy
- Acupuncture
- Surgery
Surgery is not common practice. Your doctor may suggest surgery if all the above treatments are not helping and you continue to have pain, numbness, difficulty standing or walking, and loss of bladder or bowel control.
Living with a slipped disc and managing day to day chronic pain
Living with a slipped disc can be debilitating on many levels. Doctors and pain management specialists treat all kinds of chronic pain and will come up with a plan to try to alleviate your pain and symptoms. Often your doctor may suggest physiotherapy or/and an ultrasound guided injection for the first stage of treatment. These can be very successful in the first instance and give you good long periods of a pain-free life.
Pain serves an important purpose by letting us know that we have hurt a part of our body, such as a sprained ankle or a burnt hand. But chronic pain is often more complex. People often consider pain a purely physical reaction. However, pain has biological, psychological, and emotional factors. Chronic pain can cause anger, hopelessness, sadness, and anxiety. To treat pain effectively, you must address the physical, emotional, and psychological aspects.
Treatments including medication, surgery, rehabilitation, and physical therapy, may be helpful for treating chronic pain. Psychological treatments are also an important part of pain management. Understanding and managing the thoughts, emotions and behaviours that accompany daily discomfort can help you cope more effectively with your pain. Studies have also shown that it can actually reduce pain intensity.
Sometimes it is helpful to see a psychologist for expert advice on coping with the thoughts, feelings and behaviours that go together with “living with chronic pain”.
Patients with chronic pain may be referred to psychologists by their GP or consultant. Psychologists may talk with other healthcare professionals to address both the physical and emotional aspects of pain. Treatment plans often involve teaching relaxation techniques, changing old beliefs about pain, building new coping skills, and addressing any anxiety or depression that may accompany pain. They will also be able to help make lifestyle changes that will allow you to continue with your daily activities, work, and hobbies.
Consider the following steps that can be helpful in managing chronic pain:
- Stay active – pain can lead people to stop doing the things they enjoy. It’s very important not to let pain take over your life
- Know your limits – Continue to be active in a way that acknowledges your physical limitations. Make a plan about how to manage your pain and don’t push yourself to do more than you can handle
- Stay healthy – try low-impact exercise such as stretching, yoga, walking, and swimming. Know your capabilities.
- Distract yourself – on a painful day find ways to distract your mind. Watch a movie, take a walk, or engage in a hobby. Pleasant experiences can help you cope with pain.
- Don’t lose hope – with the right psychological treatments, many people learn to manage their pain, think of it in a different way, and take back control of their lives.
How physiotherapy can help your pain
We will do whatever we can to get you on the fastest route to recovery. Some of the treatment methods we use include:
- Mobilisation
- Strengthening exercises
- Myofascial trigger point release
- Pilates
- Cross-friction massage
- Stretching and range of movement exercises
- Acupuncture
- Functional exercises
- Kinesio-taping
