What is rheumatoid arthritis?
Rheumatoid arthritis is an autoimmune disorder that can cause incredible pain, stiffness, and swelling in your joints. Rheumatoid arthritis is a long-term condition that can be treated effectively with physiotherapy and medication. The periods of time when your symptoms become worse is known as a “flare up” and can be very painful.
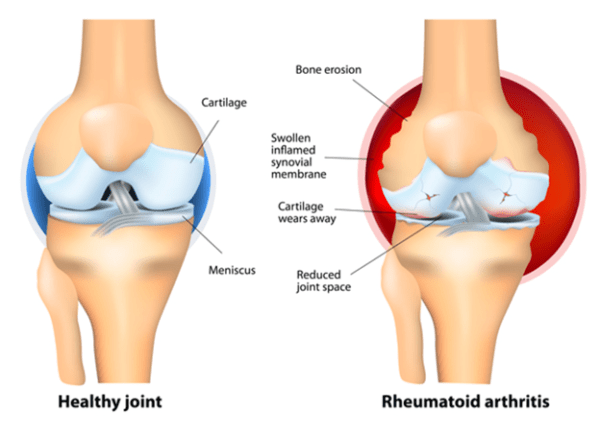
A speedy diagnosis from your doctor is crucial because early treatment can help prevent the condition getting worsening and reduce the risk of further problems, especially joint damage. Rheumatoid arthritis is usually, but not always, diagnosed with a blood test. Seropositive rheumatoid arthritis is one type which shows up in a blood test while seronegative does not. This can sometimes mislead doctors to a wrong diagnosis. Sometimes further scans are required (such as PET scans) to confirm the condition.
Rheumatoid arthritis generally affects the hands, feet, wrists, elbows, knees, and ankles. The joint effect is usually symmetrical so if one foot has it usually the other foot will also have it.
Rheumatoid arthritis often occurs more in women than men. It is actually three times more likely women, usually starting between the ages of 30 to 60. There is a genetic and environmental component that is believed to trigger the disease, but many people with rheumatoid arthritis have no family history at all.
What are the early signs and symptoms of rheumatoid arthritis?
- Before experiencing any other symptoms, you may start to feel extremely tired and lacking energy
- You may get a slight fever. Inflammation associated with rheumatoid arthritis may cause people to feel unwell and feverish. Some people mistake this fever for an infection in the body, however antibiotics does not help reduce the fever
- Your joints may be painful even at rest periods, especially in your hands.
- You may have some joint swelling that could limit your range of movement
- You may experience some redness over your joints that are giving you the pain
- Your joints will become very stiff for long periods of time and you will find it hard to mobilise them
What causes rheumatoid arthritis?
Doctors do not know exactly what causes rheumatoid arthritis. But the follow are considered a risk factor:
- Age
- Family history
- Environment
- Gender
- Obesity
- Smoking
How is rheumatoid arthritis diagnosed?
A physiotherapist may ask you a number of questions to assist in their diagnosis. These include:
- How long have you had the pain?
- Have you injured that particular joint before?
- Is it one joint or several that are painful?
- Is your joint ever stiff, especially in the mornings, and does the stiffness wear off with movement?
- Family history
- Is there any swelling? Is it in both sides/both hands?
- Is there any redness?
- Does your pain ease with rest or is it there constantly?
- How does the pain affect your daily life?
- Have you had any recent blood tests?
- Is there any history of high temperature?
- Do you suffer from fatigue?
These questions together with a physical examination aids your physiotherapist in diagnosing rheumatoid arthritis and determining a treatment plan. If rheumatoid arthritis is a potential diagnosis, your physiotherapist will refer you back to your GP or directly on to a rheumatologist prior to providing any further treatment.
How is rheumatoid arthritis treated?
The best treatment for rheumatoid arthritis include:
- Taking medication prescribed by your rheumatologist: DMARDS, Steroids, Biological treatment
- Find a balance between resting and moving the joint
- Using support for your joint such as a bandage, tubigrip, brace, or splint
- Keeping your joints warm. If it is your hands, try moving them in warm water.
- Wearing gloves outdoors
- Taking some painkillers or anti-inflammatory medication as needed
- Losing weight if the joint affected is in your legs or spine
- Adapting your day to day activities to avoid aggravating it further
- Physiotherapy to ensure you do not lose range of movement and strength
- Using a walking aid if your lower limbs are affected
- Hydrotherapy
- Steroid injections
- Doing some finger exercises if your hands are stiff. Making shapes with putty can help
- Moving your hands in warm water
- Surgery if needed to repair joints
What is the difference between osteoarthritis and rheumatoid arthritis?
Although rheumatoid arthritis and osteoarthritis both affect your joints and can be very painful, they are very different forms of the same condition. Rheumatoid arthritis is an autoimmune condition while osteoarthritis is a degenerative joint condition. Osteoarthritis is often related to a joint being overused and degenerating over time, especially with age.
Rheumatoid arthritis occurs when the immune system goes into overload and the white blood cells start to attack their own joints. Medication is often required to control the immune system overdrive and this will be prescribed by a rheumatologist. Common medication includes steroids and methotrexate to control the condition and keep the pain and swelling at bay.
The main difference between the symptoms for both conditions is that with rheumatoid arthritis, the pain and swelling often presents itself on both sides of the body (usually starting with the hands and feet) and could last all day. With osteoarthritis, the pain eases after 30 minutes or so in the morning and once you start moving. It also usually presents itself with an initial one-sided joint pain.
People with rheumatoid arthritis are more likely to suffer more with fatigue than people with osteoarthritis.
How physiotherapy can help your rheumatoid arthritis
We will do whatever we can to get you on the fastest route to recovery. Some of the treatment methods we use include:
- Mobilisation
- Strengthening exercises
- Myofascial trigger point release
- Pilates
- Cross-friction massage
- Stretching and range of movement exercises
- Acupuncture
- Functional exercises
- Kinesio-taping
