What is osteoarthritis?
Arthritis is a collective term for a broad range of conditions which ultimately causes destruction of the joint. The most common form of arthritis is osteoarthritis, however there are other conditions such as rheumatoid arthritis, psoriatic arthritis, and juvenile idopathic arthritis.
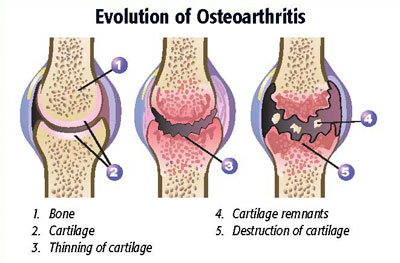
Osteoarthritis (also known as degenerative joint disease) is a breakdown of the cartilage of the joints. Sometimes it can produce bony spurs called osteophytes that can result in very painful symptoms. This is usually picked up on an X-ray or scan. The reason why osteoarthritis is so prevalent is due to the joint cartilage which has such a poor blood supply that it lacks the natural ability to repair itself. This subsequently results in more joint damage.
In most cases, treatment of osteoarthritis is geared towards relieving the symptoms of pain and increasing the ability to function. Physiotherapy plays a vital role for someone with this condition.
The 5 stages of osteoarthritis:
Stage 0 – this represents a normal knee joint
Stage 1 – minor bone spurs shown on X-ray. This is very minor wear and tear.
Stage 2 – greater bone spurs evident on X-ray but the cartilage remains in good condition. The space between the bones are normal, however you might start experiencing some intermittent pain when you are walking long distances, running, or kneeling.
Stage 3 – This is considered to be moderate osteoarthritis, where there is significant damage evident within the joint. The space between the joint begins to narrow and there would be obvious bony spurs shown on your X-ray. The fluid within the joint (the synovial fluid) may increase resulting in joint swelling and inflammation. You are likely to experience more frequent pain at this stage with regular daily activities.
Stage 4 – At this stage the osteoarthritis is severe and a knee joint replacement is often required. The joint space is likely to be minimal, leaving the bones to rub against each other. The knee joint is likely to be stiff, particularly first thing in the morning or when you are not moving for some time. You may have broken-off cartilage floating within the synovial fluid, possibly resulting in the knee catching or giving way. At this stage, your knee is likely to be very painful during most of your activities.
What are the early signs for osteoarthritis?
- Your joint may be painful mainly when moving it or putting pressure through it
- Your joint pain may ease with rest
- You may have some joint swelling and this could limit your range of movement
- Your knee may be stiff in the mornings or at times throughout the day when you are not moving for a period of time
- You may have creeking noises (crepitus) that are felt and heard
- Your knee may feel unstable and possibly give way on you
- Your may feel weakness around the knee as you begin to rely on the other leg
What causes osteoarthritis?
- Often age-related
- Previous trauma to the joint
- Being overweight
- Job involving heavy manual handling or repetitive movements
- Genetic defect
How is osteoarthritis diagnosed?
A physiotherapist may ask you a number of questions to assist in their diagnosis. These include:
- How long have you had the pain for?
- Have you injured that joint in the past?
- Is it one joint or several joints that are affected?
- Is your joint ever stiff particularly in the mornings and does the stiffness wear off with movement?
- Is there any swelling?
- Do you feel or hear any creeking?
- Is your pain dull or an ache?
- Do you get pain upon movement?
- Does your pain ease with rest?
- How is it affecting your daily life?
These questions together with a physical examination helps your physiotherapist to diagnose osteoarthritis and determine a treatment plan. However some people choose to have an X-ray or scan to clarify their diagnosis. They can then consider the intervention required moving forward.
How is osteoarthritis treated?
The best treatment for osteoarthritis includes the following:
- Find a balance between resting and moving the joint
- Use a support for your joint such as with a bandage, tubigrip, brace, or splint
- Keep your joint warm – heat therapy such as hot water bottles helps
- Exercise your joint to ensure you maintain its range of movement and strength
- Take some painkillers if need be
- Rub creams or gels containing a non-steroidal anti-inflammatory (NSAID) medicine
- Lose weight if the joint affected is in your legs or spine
- Adapt your daily activities to avoid aggravating it further
- TENS machine
- Physiotherapy
- Use a walking aid if your lower limbs are affected
- Improve your posture
- Consider complimentary therapies such as acupuncture
- Take Glucosamine and fish oil tablets
- Hydrotherapy
- Weight loss
- Steroid injections
- Joint replacement
What is the difference between osteoarthritis and rheumatoid arthritis?
Although rheumatoid arthritis and osteoarthritis both affect your joints and can be very painful, they are very different forms of the same condition. Rheumatoid arthritis is an autoimmune condition while osteoarthritis is a degenerative joint condition. Osteoarthritis is often related to a joint being overused and degenerating over time, particularly with age.
Rheumatoid arthritis occurs when the immune system goes into overload and the white blood cells start to attack their own joints. Medication, often required to control the immune system overdrive, will be prescribed by a rheumatologist. Common medication for this includes steroids and methotrexate, which is used to control the condition and keep the pain and swelling at bay.
The main difference between the symptoms for both conditions is that with rheumatoid arthritis, the pain and swelling often presents itself on both sides of the body and usually starts with the hands and feet and could, lasting all day. With osteoarthritis, the pain eases after 30 minutes or so in the morning and once you start moving. It also usually initially presents itself with a one-sided joint pain.
People with rheumatoid arthritis are more likely to suffer with fatigue than those with osteoarthritis.
How physiotherapy can help your osteoarthritis
We will do whatever we can to get you on the fastest route to recovery. Some of the treatment methods we use include:
- Mobilisation
- Strengthening exercises
- Myofascial trigger point release
- Pilates
- Cross-friction massage
- Stretching and range of movement exercises
- Acupuncture
- Functional exercises
- Kinesio-taping
