What is hypermobility syndrome?
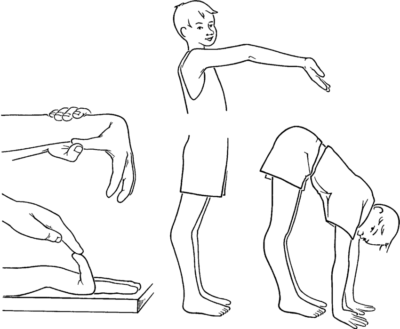
Hypermobility means that some or all joints have an unusually large range of movement. Those with hypermobility tend to be very flexible and able to move their limbs into positions that others would find unachievable. Often referred to as “loose joints” or being “double jointed”, the condition is considered advantageous for ballet dancers, gymnasts, and musicians.
Hypermobility syndrome covers a large range spectrum; from mild to severe symptoms. Ehlers Danlos Syndrome (EDS) is a much more severe case of hypermobility and can affect people in many different ways. The different types of EDS are caused by faults in certain genes that make connective tissue weaker. If you suffer from EDS you may have the following symptoms:
- Joint hypermobility
- Loose unstable joints that dislocate easily
- Clicking joints
- Extreme tiredness
- Skin that bruises easily
- Stretchy skin
- Wounds that are slow to heal
There is no test for EDS but the diagnosis is made based on medical history and physical examination.
What are the early signs and symptoms of joint hypermobility syndrome?
- Increased pain in your knees, fingers, hips, and elbows
- You have had various sprains or dislocations over time
- You hear clicking when moving your joints
- You tire very easily
- You may get digestive problems such as constipation and IBS
- You are susceptible to injury.
What causes joint hypermobility syndrome?
- Genetics
- Gender – women are more likely to have hypermobile joints
- Age
- Ethnic background
- Training/exercises
- Bone shape
How is hypermobility diagnosed?
A physiotherapist may ask you a number of questions to assist in their diagnosis. These include:
- The Beighton score – a quick measure of your flexibility using a standard set of movements
- Blood tests and scans – these may be requested
- The Brighton criteria – this takes into account your Beighton score but also considers other symptoms such as joint pain and dislocated joints
- The length of time you’ve had symptoms
- Whether it is one joint or several that are affected
- Family history
- How it is affecting you daily
These questions together with a physical examination helps your physiotherapist to diagnose hypermobility and determine a treatment plan. However, some people choose to have scans to clarify their diagnosis, eliminate other possible conditions, or assess what intervention they require moving forward. In this case, your physiotherapist may refer you back to your GP or to a rheumatologist.
How to treat joint hypermobility syndrome?
If your hypermobility does not cause daily concerns, treatment is not necessary. However, if you find you have a wide range of symptoms that do affect your daily life, the following treatments could help:
- Ensuring you have a generally healthy lifestyle and diet
- Good sleep measures
- Physiotherapy to reduce pain and improve muscle strength and fitness
- Core stability exercises
- Staying as active as you can but sticking to low impact exercises such as swimming or cycling
- Wearing comfortable and supportive footwear
- Applying heat such as a hot water bottle on painful joints
- If you have an injury from over-stretching it helps to rest the joint and elevate it
- Occupational therapy to help you overcome difficulties in your daily life
- Checking to see if you have flat feet. Orthotics can help with comfort
- Pain medication
- Relaxation techniques
- Meditation
- Splinting specific painful joints
What is the prognosis for those affected by joint hypermobility syndrome?
As joint hypermobility syndrome is a condition when the ligaments are stretched, it can predispose some individuals to wear and tear of the joints at an earlier age. Traumatic injuries are more likely to be sustained, such as sprained ankles or sprained wrists. Hypermobility syndrome itself is not a degenerative condition and there are no long-term consequences. It is simply a case of being aware they have the condition, regardless of whether they are in pain. They also need to try to avoid or minimise any traumatic events or injuries.
How physiotherapy can help joint hypermobility syndrome
We will do whatever we can to get you on the fastest route to recovery. Some of the treatment methods we use include:
- Mobilisation
- Strengthening exercises
- Myofascial trigger point release
- Pilates
- Cross-friction massage
- Stretching and range of movement exercises
- Acupuncture
- Functional exercises
- Kinesio-taping
